We support all those involved in the delivery and management of services in health and social care:
- In dealing with a variety of problems, e.g., capacity planning, demand forecasting, service redesign, patient risk profiling, performance management…
- At different decision levels: policy, strategic, tactical, operational;
- Using techniques such as stochastic modelling, simulation, statistics, data mining, data warehousing…
- In areas like A&E and urgent care, neonatal intensive care, chronic conditions, long-term care, mental health, risk prediction, performance …
PhD Project Areas 2022:
Explainable and Fair Artificial Intelligence (AI) for End-Users with Complex and Social Care Health Needs
A Blockchain Approach for Sharing and Analysing Patient Data
Supply Chain analytics: a Framework Integrating Machine Learning with Blockchain Technology
An Ethical AI Framework to Predict and Inform Risk Classification (Zoning) for Mental Health Patients
An Operational Research and AI Modelling Framework to Reduce Waiting Times for Mental Health Services
Some or our previous projects:
In order to help local councils in managing their data input to FLoSC, FLoSC-PAD (FLoSC– Preparation & Analysis of Data), a spreadsheet tool, was created.
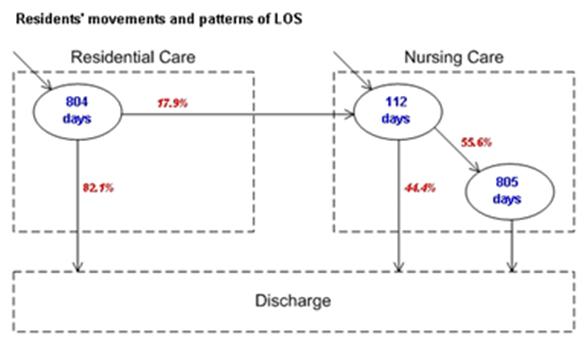
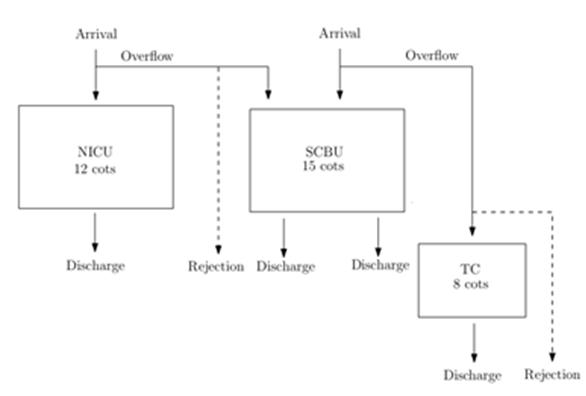
Towards effective capacity planning in a perinatal network centre: Neonatal care is provided in specialist units that are graded into three levels set by the British Association of Perinatal Medicine (from the least intensive and most common care unit to the most intensive). First, the arrival pattern and length of stay (LoS) in the care units (i.e. neonatal intensive care/high dependency unit (NICU/HDU) and special care baby unit (SCBU)) were studied. Then, the impact of capacity shortage in a perinatal network centre was estimated and analytical models for improving capacity planning were provided. Finally, a simulation model was developed to evaluate the performance of the perinatal network.
Forecasting patient demand for NHS continuing healthcare: First problem structuring methods were used to identify existing practices relating to demand management in NHS continuing healthcare and how such work fed into related workstreams – including early contracting negotiations with private sector providers. Based on the need to integrate with existing data systems and provide a streamlined way for commissioning teams to generate forecasts based on changes in several factors – we developed an online web-based forecasting system which could be used to generate graphs and reports of future spend and demand for care across six categories of care and under different provision types and future scenarios.

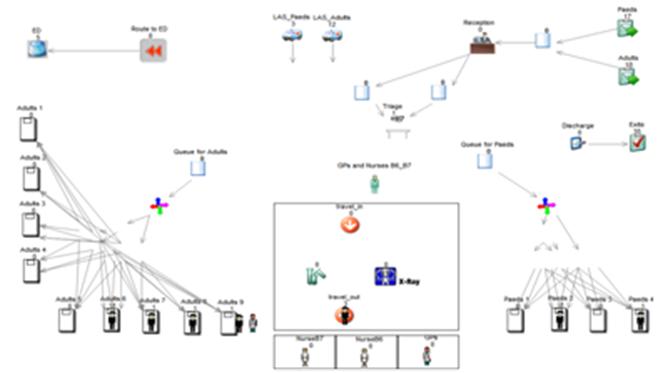
Urgent Care services redesign: As part of a Knowledge Transfer Partnership project, using data mining techniques, we developed an understanding of system behaviour in terms of subsystem interactions and the factors influencing patient flows. The insight obtained through Clustering analysis and Association Rules mining was then used as patients’ demand and pathways supporting better services in the UCC. Previous A&E attendances data have been clustered into groups and sub groups on their resources used and acuity. These groups are the identified target groups for service specification strategy design and decision making process.
In order to make a strategic business decision with confidence, we developed a Simulation model that captures most of the details generated by the clinical model down to operational planning, such as determining appropriate Nurse and Doctors staffing levels and monitoring performance metrics for the UCC.
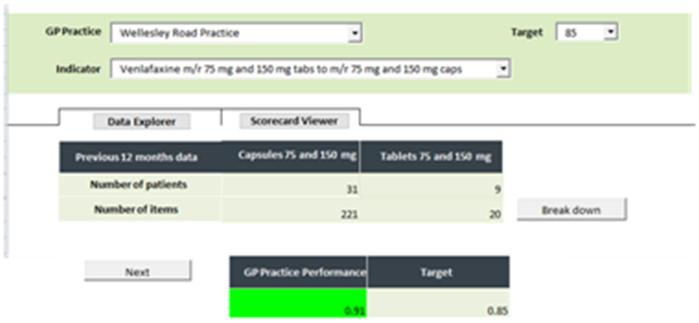
Prescribing dashboard and case management prescribing benchmarker: As part of Knowledge Transfer Partnership project between NHS Hounslow and University of Westminster a data warehousing and business intelligence solution is proposed to improve prescribing performance monitoring and analysis in NHS Hounslow. An executive Prescribing Dashboard is built to support managerial decision making, which is critically dependent on integrated information presented in timely and easily understood manner, while a Medicines Management Benchmarker is built to assist clinicians with assessing whether prescribing is clinically appropriate and cost effective.
